Neuroscience class takes learning into operating room at Carilion Roanoke Memorial Hospital
The School of Neuroscience at Virginia Tech’s Clinical Neuroscience in Practice course is no ordinary class.
It offers undergraduate students the opportunity to experience the world of a neurosurgeon, both in the classroom and the operating room.
In class, students receive lectures from residents and attending physicians from Carilion Roanoke Memorial Hospital and get to ask questions and see real-life clinical cases and treatments.
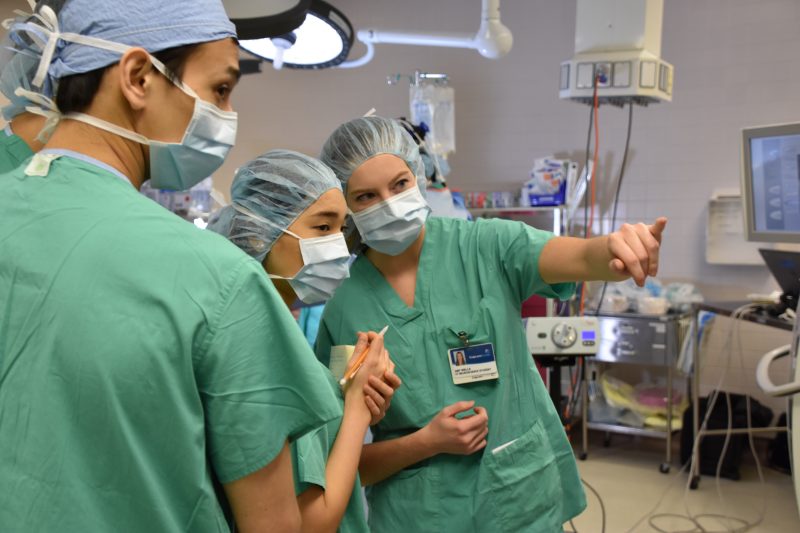
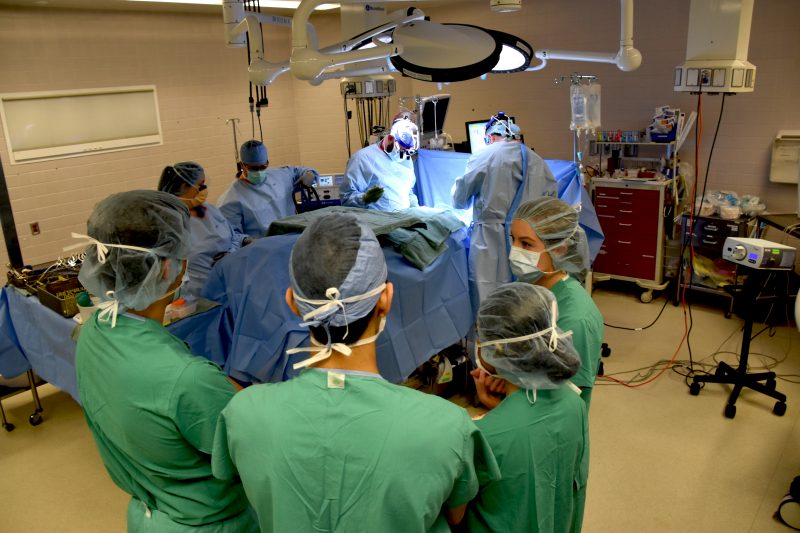
Students go into an operating room to watch brain and spine surgery – scrubs on, notebooks in hand – at Carilion Roanoke. Students can also follow residents on patient rounds and stay two nights “on-call” to witness medical emergency care first-hand.
The experiences are one of a kind.
“I keep telling the students every single time we come here, this is not normal, you are seeing a neurosurgery team opening their world to undergraduates,” said Harry Sontheimer, I.D. Wilson Chair and professor of neuroscience and executive director of the School of Neuroscience, part of the Virginia Tech College of Science.
The neuroscience course is a collaboration between Virginia Tech and Roanoke-based Carilion Clinic, which already has resulted in the Virginia Tech Carilion School of Medicine and Research Institute.
Eighteen students are enrolled in the spring 2017 Clinical Neuroscience in Practice class. Among them is Amy Wells, of Melbourne, Florida, a senior double majoring in psychology and neuroscience in the College of Science, and Tariq Ayubi, of South Riding, Virginia, a junior double majoring in biological sciences and biochemistry in the College of Science and the College of Agriculture and Life Sciences, respectively.
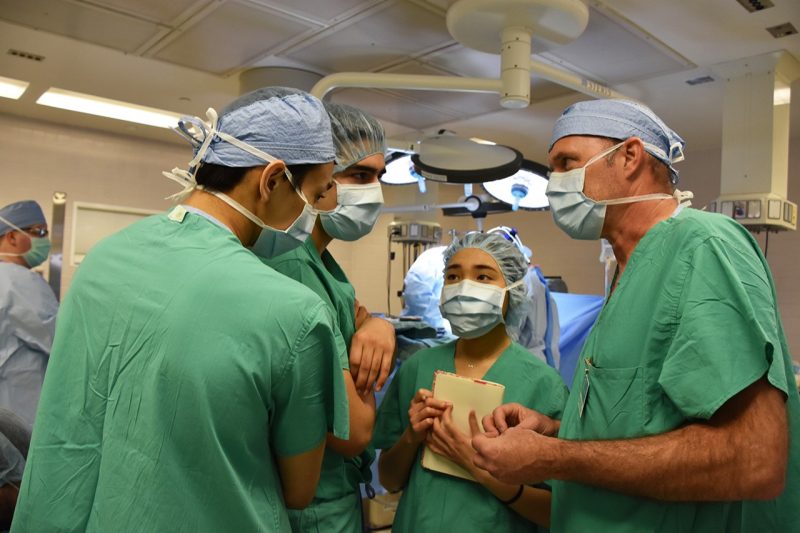
Recently, Wells and Ayubi watched a neurosurgery team led by Carilion neurosurgeon Lisa Apfel, who is also assistant professor of surgery at the Virginia Tech Carilion School of Medicine. Before the surgery, Apfel briefed Wells, Ayubi, and two other undergraduate students on the patient’s history and what would happen during and after the surgery.
“I am a very visual learner, and for me to see the cases and see what is happening, that is a very big learning tool for me,” Wells said. “A lot of the time what you see in textbooks can be very different from what you see in person. Having [Dr. Apfel] go through the pictures and describe what they are doing is incredibly helpful.”
(Note: Patients or their families give permission to Carilion allowing students to watch a surgery. Permission for photography was also was given to Virginia Tech.)
Wells, who has wanted to enter medicine since childhood, has witnessed surgeries before. Ayubio on the other hand, was seeing his first.
“I woke up at 5:30 this morning, and I have never felt so energized in my life,” he said while standing outside the operating room as Carilion medical personnel hustled to and from operating rooms.
After spending time in the operating room, Ayubio said he felt lucky to be able to take the course.
"I’ve been able to watch several surgeries and have seen the [neurosurgery] team do amazing things," he said. "During the surgeries, I am usually able to stand by the anesthesiologist and have a fairly decent view of what is going on.”
In the classroom at Virginia Tech, students learn about various types of cases, including stroke, trauma, spinal cord injuries, brain tumors, and more. It is not all lecture.
Sontheimer and residents ask students how they would treat a case or ask vital questions such as, “How do you tell a person that they have cancer?”
Gary Simonds, chief of neurosurgery at Carilion and professor of surgery at the Virginia Tech Carilion School of Medicine, and Sontheimer designed and co-lead the Clinical Neuroscience in Practice course to be all encompassing. It is Simonds who has made it possible for students to interact with and learn by the side of neurosurgeons in a hospital setting.
“It is such a fantastic opportunity to be around people like the people at Tech and, hopefully, they feel the same way with us and this creates that bridge,” Simonds said. “For us, and particularly for our residents, we feel that the better a physician is as an educator, the better they are as a physician.”
Sontheimer said the experience of students being on call overnight at the side of neurosurgeons is especially transformative and an ideal showcase for experiential learning. For instance, students learned the landing of helicopters at the hospital could mean a brain or spinal cord injury.
“When this happens, neuroscience students are truly in the midst of the exhaustive efforts to save people’s lives,” Sontheimer said. “This is the real deal, not a scripted episode of some medical drama.”
Ethics are also discussed, as is the well-being of patients and their families.
“Is surgery better than the natural course or medicine we can be using,” asked Simonds of his students during one class.
Not all the students in the class will go onto become neurosurgeons. In fact, few will, Sontheimer said. Most may become practitioners or biologists or lawyers.
Sontheimer has called neuroscience “the new English major.” Just as getting a grounded education in English can the foundation of dozens of careers, so can neuroscience.
“Clearly, this gives us an opportunity to do something in clinical neuroscience that wouldn’t be possible without Carilion,” Sontheimer said.
For the students, whether or not they go into medicine the impact is immeasurable.
“Dr. Simonds and Dr. Sontheimer have been incredible mentors. I don’t think you could ask for better faculty to be involved with. They are very much about making sure students have the opportunity to learn and that the learning they do is meaningful,” Wells said, before heading back into the operating room.